Email us:
info@andrea-digestive-clinic.comCall us:
+65 6264-2836#21-11/12 Royal Square Medical Centre
Mon - Fri : 9am - 5pm, Sat : 9am - 1pm
Haemorrhoids, also known as piles, are part of the anal canal. Piles can cause problems when they become enlarged, swollen, inflamed or bleeding and cause pain around the anus. Under the normal circumstances, piles act as cushions composed of vessels and surrounding tissue that aid the passage of stool.


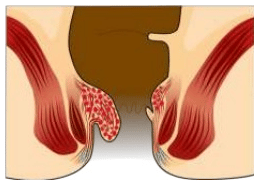
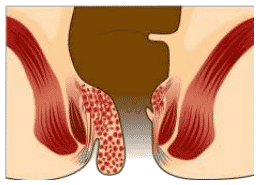

There are two types of piles (external and internal) which are differentiated via their position with respect to the dentate line.
External haemorrhoids are those that occur outside and around the anus. Symptoms include occasional pain, and they are often accompanied by swelling and irritation. Itching, although often thought to be a symptom of external piles, is more commonly due to skin irritation. External piles are prone to thrombosis. This happens if the vein ruptures and/or a blood clot develops within the haemorrhoid.
Internal haemorrhoids are those that occur inside the rectum, and are not visible outside the anus. Internal piles are usually without pain and generally have few noticeable symptoms. Most people are not aware that they have them. Internal piles, however, may bleed when irritated or enlarged. Normally, the bleeding is limited to small stains of fresh blood on the toilet paper, but more severe bleeding may occur during passing a hard stool. When internal piles are large, they may prolapse outside the anus.
Internal piles can be further graded by the degree of protrusion from the anus (prolapse). Pictures are taken during the endoscopy.

Haemorrhoids are very common in both men and women. About half of the population have piles by age 50.

A number of factors may lead to the formations of haemorrhoids including irregular bowel habits, constipation, diarrhoea, exercise, pregnancy, nutrition (low-fiber diet), increased intra-abdominal pressure (prolonged straining), obesity, sitting for long periods of time and aging.
How are haemorrhoids prevented?
The best way to prevent piles is to keep stools soft so they pass easily, thus decreasing pressure and straining and to initiate bowel movement as soon as possible after the urge occurs. Exercise including walking, high fibre diet and adequate water intake help reduce constipation, regulate bowel movements and straining by producing stools that are softer and easier to pass.
A thorough evaluation and proper diagnosis is important any time bleeding from the rectum or blood in the stool occurs. Bleeding may also be a symptom of other digestive diseases, including colorectal cancer.
Anus and rectum will be will examined for swollen blood vessels that indicate piles. A digital rectal exam will be performed to feel for abnormalities, such as colorectal cancer. Closer evaluation of the rectum for piles requires an exam with a proctoscope, a hollow tube useful for viewing internal haemorrhoids.
To rule out other causes of gastrointestinal bleeding, the entire colon will be examined with colonoscopy.


1. Lifestyle Modifications
Small haemorrhoids can get better even without medical treatment. Piles, if they are caused by constipation or poor bowel movements, the aim of the treatment is to achieve regular soft stools. A softer stool and regular bowel movement makes emptying the bowels easier and lessens the pressure on piles caused by straining. The most important measurement is a change of diet with the addition of more fibre and roughage particularly green vegetables, fresh fruit, wholegrain cereals and bran. Fluid intake should be increased to 8 to 10 glasses (2L) of fluid daily.
The patient is also advised to avoid straining when passing a stool and to avoid sitting on the toilet for longer than necessary. Reducing your use of mobile devices while visiting the toilet can help reduce the time you spend in the toilet.
Sitting in a shallow bath of hot water for 15 minutes several times a day, will reduce the pain and symptoms.
2. Piles Medication
Relatively small haemorrhoids can be treated using creams applied on areas around the anus, or suppository together with medication venotonic (Daflon).
3. Rubber Band Ligation
More severe cases need to be treated by a specialist. One possible treatment is rubber band ligation. It is performed as outpatient procedure and does not require hospital admission. The procedure involves placing a small rubber band at the base of the haemorrhoid with a special applicator. The rubber band constricts the blood vessels at the location cuts off the blood supply to the haemorrhoid, which eventually falls off after a few days. Cure rate has been found to be about 87%. This technique is effective for treating moderate size haemorrhoids.
Rubber band ligation is not appropriate for treating large or bulky haemorrhoids. Piles that are previously treated with sclerotherapy are difficult to band, and therefore should not be treated with this procedure.
If the piles/haemorrhoids are too large and they protrude through the back passage and cannot be manually reduced, the treatment requires surgical removal or ‘haemorrhoidectomy’. Following any treatment for piles, it is very important to avoid constipation and straining or the condition may recur.
Find out more about Haemorrhoids/Piles Treatment at Andrea's Digestive Clinic.

