Email us:
info@andrea-digestive-clinic.comCall us:
+65 6264-2836#21-11/12 Royal Square Medical Centre
Mon - Fri : 9am - 5pm, Sat : 9am - 1pm
Celiac disease is an immune-based reaction to dietary gluten (storage protein for wheat, barley, rye) which affects the small intestine in those with a genetic predisposition and resolves with exclusion of gluten from the diet. There has been a substantial increase in the prevalence of celiac disease over the last 50 years and an increase in the rate of diagnosis in the last 10 years.
Celiac disease is one of the most common causes of chronic malabsorption. This results from injury to the small intestine with loss of absorptive surface area, reduction of digestive enzymes, and subsequently impaired absorption of micronutrients such as fat-soluble vitamins (A,D,E,K), iron, and vitamin B12, folic acid, zinc, etc. In addition, the inflammation worsens symptoms of malabsorption by causing secretion of fluid into the intestine that can result in diarrhoea. The failure of absorption of adequate calories and nutrients leads to weight loss, and the malabsorption results in abdominal pain and bloating.


Nausea and vomiting can vary from an unsettled feeling in the stomach to the violent action of immediate vomiting. Nausea and vomiting are linked to may GI conditions and also to some non-GI disorders.
Bloating can result from excessive gas in the digestive system due to fermentation and swallowing air while eating or failure of the digestive tract to break down nutrients into small absorbable molecules (e.g lactose intolerance or celiac diseases).
Constipation is the decreased frequency or slowing of peristalsis, resulting in harder and infrequent stools. When the GI tract is slowed down, faeces can accumulate in the colon with attending pain and bloating. It is often result of inadequate water and fiber intake and increased intake of processed and fatty food.
Diarrhoea is the increased frequency of bowel movements, which are also loose or watery. Diarrhoea could be associated with food allergy or celiac disease, but is also present in other inflammatory bowel conditions or irritable bowel.
Abdominal pain appears in different patterns and with varying intensities. It is a common symptoms of various GI problems.

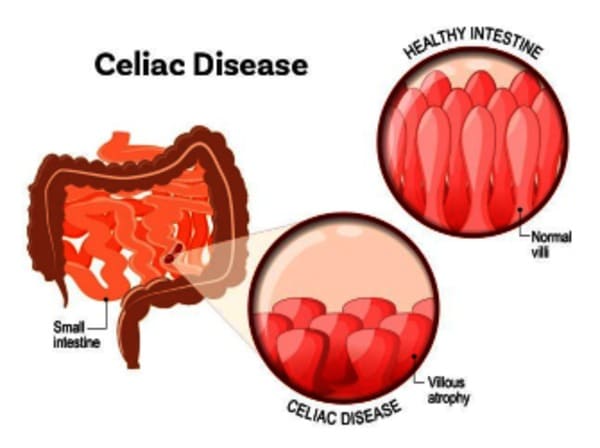
Celiac disease is usually detected by blood test – testing of specific gene carrying the predisposition and celiac-specific antibodies. The diagnosis is confirmed by small intestine (duodenal) mucosal biopsies taken during gastroscopy. Both blood test and biopsy should be performed when patient is taking gluten containing diet. When someone is on gluten-free diet, antibodies blood test and biopsies could be only done after daily exposure to gluten for at least 3 weeks.
The treatment for celiac disease is primarily a gluten free diet, which requires significant patient education, motivation, and follow-up. Speak to out nutritionist, Veronica Cavallini at our clinic to find out more.
